Bilevel positive airway pressure machines, also known as BiPAP or BPAP devices, use a stream of pressurized air to treat sleep apnea. A BiPAP machine delivers air at a higher pressure when you are breathing in and at a reduced pressure when you are breathing out.
Although they are less commonly used than CPAP and APAP devices, BiPAP machines can offer benefits to certain people with obstructive sleep apnea, central sleep apnea, and other other conditions that affect nighttime breathing.
How Does BiPAP Work?
Like other positive airway pressure (PAP) treatments, BiPAP therapy uses a machine to force pressurized air into the upper airway. This flow of air keeps the airway open during sleep to facilitate uninterrupted breathing. A BiPAP machine delivers air at two different pressure levels, one when breathing in and another when breathing out.
- Inspiratory positive airway pressure (IPAP): The term IPAP refers to the level of air pressure provided by a BiPAP device while you are inhaling. With BiPAP therapy, the IPAP level is higher than the pressure during exhalation.
- Expiratory positive airway pressure (EPAP): EPAP is the level of air pressure delivered by the device during exhalation. When using a BiPAP machine, the EPAP level is lower than IPAP, which means you breathe out against a less forceful flow of air.
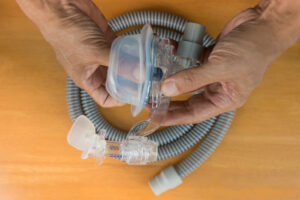
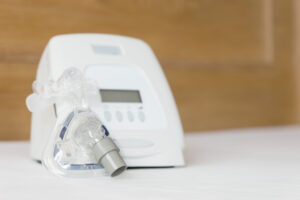
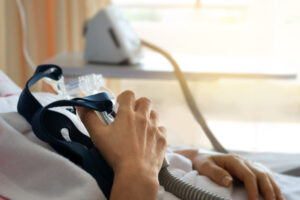
BiPAP therapy uses a small bedside machine that pressurizes air and pumps it through tubing. The tubing is attached to a mask worn over either the nose or both the nose and mouth. The pressurized air enters through the mask and flows into the upper airway.
BiPAP machines can operate in different modes. In spontaneous mode, the BiPAP machine switches between IPAP and EPAP levels based on your breathing. In timed mode, the machine delivers air on a set schedule. In spontaneous/timed (S/T) mode, the machine will send a stream of air if it detects that you have not initiated a breath after a certain amount of time. A doctor will determine which mode is most appropriate in your situation.
In many cases, the pressure settings for a BiPAP machine are set in advance by your doctor. However, some BiPAP machines have sensors that track your breathing and adjust pressure levels in real time. These are called auto-titrating or auto-adjusting BiPAP machines.
BiPAP vs. CPAP
Both BiPAP and continuous PAP (CPAP) devices use pressurized air to support more consistent breathing in people with obstructive sleep apnea and other breathing disorders. However, CPAP provides a fixed level of air pressure, while BiPAP provides different pressure levels during inhalation and exhalation.
CPAP and BiPAP have a number of similarities, and both can be effective treatments for sleep apnea. That said, there are important differences between CPAP and BiPAP machines.
With a BiPAP device, lower air pressure during exhalation can make exhaling more comfortable. This can be especially advantageous for people whose treatment requires a high level of air pressure during inhalation.
However, BiPAP machines are rarely used as an initial treatment for obstructive sleep apnea in people without other breathing difficulties. With their ability to operate in many different modes, BiPAP devices may be better suited to treat complex breathing problems, such as when a person has both obstructive and central sleep apnea.
BiPAP machines tend to be more expensive than CPAP devices, and there may be fewer options available for travel BiPAP devices.
What Is a BiPAP Machine Used For?
For obstructive sleep apnea, BiPAP devices are not widely used for initial treatment. Instead, BiPAP therapy is generally prescribed if prior treatment with a CPAP or APAP machine was not beneficial. BiPAP therapy may also be suggested for people who have obstructive sleep apnea alongside another breathing disorder like central sleep apnea.
Because it can be programmed to deliver air at regular intervals, BiPAP treatment can be used to normalize the breathing patterns of people with more complex conditions that may cause breathing during sleep to be irregular, too shallow, too slow, or too deep.
These conditions include:
- Central sleep apnea
- Obesity hypoventilation syndrome
- Chronic obstructive pulmonary disease (COPD)
- COVID-19 and respiratory failure
Who Is BiPAP Best For?
BiPAP therapy should only be used by certain people with sleep apnea and other breathing disorders. In people with obstructive sleep apnea, BiPAP therapy is normally only used in select circumstances.
- Ineffectiveness of other PAP therapy: BiPAP therapy may be appropriate if obstructive sleep apnea does not improve after trying treatment with a CPAP or APAP machine.
- Discomfort with CPAP: People who have trouble sticking with their CPAP treatment because they are uncomfortable exhaling against the incoming air pressure may benefit from trying a BiPAP device.
- Other coexisting breathing issues: BiPAP devices may be prescribed for people who have obstructive sleep apnea along with another condition that interferes with consistent breathing, such as central sleep apnea, obesity hypoventilation syndrome, muscular dystrophy, or stroke.
In any specific situation, a doctor or sleep specialist can help determine if BiPAP therapy is appropriate. A prescription is required in order to obtain and use a BiPAP device.
What are the Benefits of BiPAP?
Like other forms of PAP therapy, BiPAP treatment can potentially resolve sleep apnea and other sleep-related breathing problems. Benefits of effective treatment may include:
- Improved sleep with fewer unwanted awakenings
- Less daytime sleepiness
- Clearer thinking and improved memory
- Better mood
- Improved control of blood pressure
- Reduced snoring
- Lower risk of cardiovascular problems and other health complications associated with untreated sleep apnea
What are the Risks of BiPAP?
There are few safety risks associated with PAP therapy, but some side effects are common, especially at the start of treatment. It is helpful for people who begin using a BiPAP machine to work with their doctor to troubleshoot side effects during the first few weeks.
Common side effects can include:
- Nasal congestion, runny nose, or upper respiratory infections
- Skin irritation from the mask
- Dry mouth
- Feelings of claustrophobia
- Nosebleeds
When side effects occur during BiPAP treatment, there are often steps that can help manage them. Changing the mask, adding a humidifier, adjusting settings, ensuring equipment is cleaned properly, and other practical steps can frequently eliminate uncomfortable side effects.
What to Expect Before Using a BiPAP Machine
Before you start BiPAP therapy, it is common for the device to be set up during an overnight sleep study. During the study, your health care provider or a sleep technician can help you select a comfortable mask and adjust the pressure settings on the BiPAP machine.
You will receive a user’s manual and instructions on how to operate and clean your machine. It usually takes a few weeks to get used to using a PAP device. Be sure to communicate with your health care team if you have any problems using your device. Your doctor or sleep technician can often suggest changes to make BiPAP therapy more convenient and comfortable.
As you get started, taking certain steps may help you more quickly get used to BiPAP treatment.
- Make sure you are wearing the mask correctly: Test the mask for comfort, making sure it is neither too loose nor too tight. When worn properly, you should not hear air leaking out of the mask.
- Practice while you’re awake: Put on the mask and turn on the machine while you’re reading or watching TV to get used to how it feels. Take notes about any discomfort or other issues so you can review them with your health care provider.
- Set up a routine for cleaning your machine: Cleaning your BiPAP device regularly helps keep it operating properly and reduces unwanted exposure to germs.
- Be patient: It’s normal for it to take time to adjust to using PAP therapy at night, so don’t give up if you encounter challenges. It’s important to follow up with your doctor to troubleshoot and make adjustments.
References
Ask the Sleep Doctor
Have questions about sleep? Submit them here! We use your questions to help us decide topics for articles, videos, and newsletters. We try to answer as many questions as possible. You can also send us an email. Please note, we cannot provide specific medical advice, and always recommend you contact your doctor for any medical matters.