On This Page
Obstructive Sleep Apnea
Our editorial process includes extensive measures to verify accuracy, provide clarity on complex topics, and present factual information. Read more
Key Takeaways
- Obstructive sleep apnea is a common sleep disorder in which the airway narrows or closes during sleep, causing breathing pauses that can lower oxygen levels and fragment sleep.
- Symptoms may vary but can include loud snoring, choking or gasping during sleep, non-refreshing rest, daytime fatigue, difficulty concentrating, and mood changes.
- OSA is typically diagnosed with a sleep study, which can be performed in a sleep lab or at home. Sleep Doctor offers simply at-home sleep testing option.
- The most common treatment options include positive airway pressure (PAP) therapy and oral appliances. Sleep Doctor can help guide patients through treatment options.
What Is Obstructive Sleep Apnea?
Obstructive sleep apnea is a sleep disorder in which a person’s airway repeatedly narrows or closes during sleep, limiting or completely blocking airflow. These obstructions occur when the muscles in the throat relax too much, allowing soft tissues to collapse into the airway.
As breathing becomes restricted or briefly stops, the brain sends a signal that partially wakes the sleeper so breathing can resume. These brief awakenings often happen dozens of times per hour, even if the person doesn't fully remember them, leading to fragmented sleep and reduced sleep quality.
Because the airway obstruction occurs during sleep, many people are unaware they have the condition until a bed partner notices symptoms such as loud snoring, choking, or gasping for air.
Central vs. Obstructive Sleep Apnea
OSA is one of two types of sleep apnea. The other type, called central sleep apnea (CSA), also involves repeated pauses in breathing.
However, in central sleep apnea, breathing stops because the brain doesn't consistently send signals to the muscles that control breathing. CSA is less common and is more often linked to underlying medical conditions, such as heart failure, stroke, neurological disorders, or the use of certain medications.
Some people have a combination of both types, known as complex or mixed sleep apnea. Because the causes differ, diagnosis and treatment approaches may also vary, making proper evaluation important.
What Are Symptoms of Obstructive Sleep Apnea?
The symptoms of obstructive sleep apnea vary from person to person. While some people have no symptoms or are unaware of them, the the most common OSA symptom is snoring.
Around 80% to 90% of people with obstructive sleep apnea snore, but not everyone who snores has OSA. A doctor’s assessment is the only way to tell if snoring is caused by OSA. If someone in your life shows signs of sleep apnea, talk to them about seeking an assessment from a medical professional.
Additional signs and symptoms of obstructive sleep apnea include:
- Loud snoring, gasping, or choking
- Restless or unrefreshing sleep
- Excessive daytime sleepiness
- Realistic, odd, or scary dreams
- Waking up at night needing to urinate
- Choking, gasping, or snorting during sleep
- Morning headaches
- Difficulty concentrating
- Mood changes
While obstructive sleep apnea can’t be diagnosed based on symptoms alone, recognizing symptoms can be a crucial step to getting medical care. If you’re unsure about your own nighttime breathing, talk to a bed partner, roommate, or caregiver about whether they have noticed any concerning signs while you sleep.
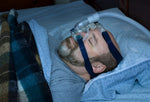
When you lie on your back all of the anatomy falls to the back of the throat. What happens? It makes the airway more narrow, which makes the air move faster, which makes it easier to vibrate the muscles. If it gets even worse, it causes an obstruction and sleep apnea.
Obstructive Sleep Apnea in Children
The symptoms of sleep apnea in children can be different from adults. Parents and caregivers who are concerned about their child’s nighttime breathing should also take note of loud or frequent snoring. But other signs and symptoms of obstructive sleep apnea in children include:
- Sleepwalking
- Bedwetting
- Sweating while asleep
- Learning difficulties
- Hyperactivity
- Aggression
What Causes Obstructive Sleep Apnea?
Obstructive sleep apnea is caused by blockages in the airway during sleep. As a person falls asleep, the tissues in their mouth and throat begin to naturally relax, which can reduce the space in their airway. Normally, these changes are of little consequence and don’t affect a person’s breathing pattern, oxygen levels, or sleep.
But for people at risk of obstructive sleep apnea, these natural changes in the throat can cause the airway to become blocked, either partially or completely. Blockages can last for a few seconds to a minute or more, causing the sleeper to wake up in order to breathe.
Risk Factors for Obstructive Sleep Apnea
Although anyone can develop this condition, a variety of risk factors increase a person’s susceptibility to airway blockages and the development of obstructive sleep apnea.
- Age: After young adulthood, the risk of developing obstructive sleep apnea increases and then peaks by the time people reach their 70s.
- Sex: Males are two to three times more likely to develop obstructive sleep apnea. The risk of obstructive sleep apnea in females increases when they near or begin menopause.
- Body weight: The likelihood of developing obstructive sleep apnea increases along with a higher body mass index (BMI), which is a method of calculating body fat according to a person’s weight and height. An estimated 60% to 70% of people with OSA have obesity.
- Physical characteristics: Certain physical features, like a small jaw or large tonsils, increase the chances of obstructive sleep apnea.
- Smoking: Tobacco smoking may increase the risk of OSA and can also make breathing disruptions worse.
- Family history: The risk of obstructive sleep apnea may be higher for people with family members who snore or have OSA. This link could be related to genetics or to shared living conditions within a family.
- Nasal congestion: Having a stuffy or congested nose can double the risk of obstructive sleep apnea.
The risk of obstructive sleep apnea is also increased by conditions that affect a person’s physical health, such as pregnancy, high blood pressure, and chronic obstructive pulmonary disease (COPD).
In children, obesity and enlarged adenoids or tonsils are the main risk factors for obstructive sleep apnea. The adenoids and tonsils are tissues in the back of the throat that help combat infections. When these tissues are larger, they reduce the size of the airway and make it more prone to blockage during sleep.
How Is OSA Diagnosed?
If you're concerned about obstructive sleep apnea, talk to your doctor. An evaluation for obstructive sleep apnea typically includes questions related to a person’s symptoms and medical history. If your doctor suspects OSA based on your symptoms, they may refer you to a specialist in sleep medicine.
To diagnose obstructive sleep apnea, a sleep specialist will consider a person’s medical history and the results of a sleep study.
Sleep Study (Polysomnography)
A sleep study, conducted overnight in a specialized sleep laboratory, can confirm a diagnosis of obstructive sleep apnea. During a sleep study, a sleeper is monitored by a variety of devices that measure and record certain body functions. Measurements include breathing patterns, the level of oxygen in the blood, and sleeping position.
Alternatively, a doctor may recommend a home sleep apnea test. An at-home sleep test records fewer measurements than an in-lab sleep study but may be an option when a doctor strongly suspects sleep apnea that isn’t complicated by another medical condition.
Sleep Doctor offers an at-home sleep test that lets you collect sleep data in the comfort of their own bed. The test is mailed directly to you, includes simple instructions, and is reviewed by a qualified medical professional to help determine if you have obstructive sleep apnea.
Sleep Apnea Severity
When a doctor diagnoses obstructive sleep apnea, they classify the condition’s severity based on a person’s symptoms and apnea-hypopnea index (AHI). The AHI is the average number of disturbed breathing episodes during each hour of a sleep study.
Knowing the severity of a person’s obstructive sleep apnea helps doctors determine the best treatment. Obstructive sleep apnea may be classified as mild, moderate, or severe.
| Apnea-Hypopnea Index (AHI) | Symptoms | |
|
Mild Obstructive Sleep Apnea |
5 to 14 |
|
|
Moderate Obstructive Sleep Apnea |
15 to 30 |
|
|
Severe Obstructive Sleep Apnea |
More than 30 |
|
Complications of Undiagnosed Obstructive Sleep Apnea
Obstructive sleep apnea can lead to potentially serious consequences if left untreated. Possible complications of obstructive sleep apnea include:
- Motor vehicle accidents
- Reduced attention span and memory
- Mood changes and depression
- Sexual dysfunction
- Heart disease and stroke
- Type 2 diabetes
These complications may be caused by several factors related to sleep apnea, including the effects of sleep loss, repeated drops in the amount of oxygen in the blood, and changes in heart rate and blood pressure.
What Are the Treatments for Obstructive Sleep Apnea?
Obstructive sleep apnea is treated as a chronic condition needing long-term, nightly treatment. Treatment of OSA is aimed at restoring normal breathing, enhancing sleep quality, and relieving other symptoms.
Doctors typically recommend positive airway pressure (PAP) therapy in combination with lifestyle changes. If people aren’t able to tolerate these treatments or the treatments aren’t helping, doctors may recommend oral appliances or surgery.
Sleep Doctor's Sleep Care Advocates can help guide patients through their treatment options and next steps, following their sleep test and diagnosis. This may include education about PAP therapy, help understanding equipment and settings, and support in exploring alternatives.
PAP Therapy
Positive airway pressure therapy keeps the airway open by pumping pressurized air into the upper airway from a bedside machine. PAP therapy can reduce breathing interruptions in most people with OSA and is considered the cornerstone of treatment by sleep experts.
There are several types of PAP therapy recommended for OSA.
- CPAP: Continuous positive airway pressure (CPAP) machines supply a fixed, steady stream of air to keep the airway open.
- BiPAP: Bilevel positive airway pressure (BiPAP or BPAP) provides two levels of pressure: a higher level during inhaling and a lower pressure during exhaling.
- APAP: Auto-adjusting positive airway pressure (APAP) is a technology available on many CPAP or BiPAP machines that adjusts pressure based on a person’s needs throughout the night.
Emerging alternatives to CPAP therapy may be options for people who can’t tolerate, or don’t benefit from, other PAP therapies. One of these alternatives, called expiratory positive airway pressure (EPAP), doesn’t require a bedside machine. Instead, EPAP devices are inserted into the nostrils and help keep the airway open using pressure created by a person’s own breath.
Oral Appliances
Oral appliances for sleep apnea are devices that are inserted into the mouth to shift the jaw and tongue forward, which lowers the chances of airway blockage. There are two main types:
- Mandibular advancement devices (MADs): These appliances reposition the lower jaw slightly forward during sleep, helping keep the airway open.
- Tongue-retaining devices (TRDs): These devices hold the tongue in a forward position using gentle suction to prevent it from falling back and blocking the airway.
While these devices are less effective than CPAP in treating obstructive sleep apnea, they may be helpful for reducing snoring and treating mild OSA.
Surgery
Sleep apnea surgery can make the airway larger or prevent it from becoming blocked during sleep. Doctors may recommend surgery when other treatments aren’t helping, or if they believe surgery could make CPAP therapy more effective.
- Uvulopalatopharyngoplasty (UPPP) removes or reshapes excess tissue in the throat, such as the uvula or soft palate, to widen the airway.
- Nasal surgery corrects structural issues like a deviated septum or enlarged turbinates to improve airflow through the nose.
- Tonsillectomy or adenoidectomy removes enlarged tonsils or adenoids that may be blocking the airway, more commonly performed in children but sometimes in adults.
- Jaw surgery (maxillomandibular advancement) repositions the upper and lower jaws forward to create more space behind the tongue and soft palate.
- Upper airway stimulation therapy involves an implanted device that stimulates airway muscles to keep the airway open during sleep.
For children with obstructive sleep apnea, surgery may be the first treatment they receive. Many children have enlarged adenoids and tonsils that can block their upper airways while they sleep. Removing these tissues may keep the airway open and improve nighttime breathing.
Living With Obstructive Sleep Apnea
For many people, working with a doctor to diagnose and treat obstructive sleep apnea can provide relief from symptoms, reduce potential complications, and improve their quality of life. Because these treatments often require adjustments to daily habits, it can take time for people to get used to living with obstructive sleep apnea.
When starting CPAP therapy, it’s normal to feel uncomfortable with the mask, air pressure, or the noise from the machine. Since the CPAP machine must be used every night to be effective, people should promptly discuss any concerns or problems using a CPAP machine with their doctors.
Sleep hygiene can help anyone living with obstructive sleep apnea get sufficient and high-quality rest. Improving sleep hygiene means practicing healthy sleep habits such as:
- Setting aside enough time for sleep
- Maintaining a consistent sleep schedule
- Avoiding caffeine later in the day
- Keeping electronics out of the bedroom
- Limiting alcohol consumption
Lifestyle adjustments can also be an important part of OSA care. Exercise and weight loss may be recommended to reduce breathing issues and ease daytime symptoms. It’s also a good idea to review medication use with a doctor, as certain medications can make sleep apnea worse.
Frequently Asked Questions
Can obstructive sleep apnea be cured?
Obstructive sleep apnea is usually considered a chronic condition, meaning it often requires ongoing management rather than a one-time cure. In some cases, such as after significant weight loss or corrective surgery, symptoms may improve substantially or even resolve. However, many people continue to need treatment.
Is obstructive sleep apnea a disability?
Obstructive sleep apnea can be considered a disability in certain circumstances, particularly if it significantly interferes with daily functioning or the ability to work. In the United States, OSA may qualify as a disability for workplace accommodations or disability benefits if symptoms are severe, well-documented, and not adequately controlled with treatment. Eligibility depends on individual circumstances and applicable laws or employer policies.
Is OSA dangerous?
Yes, untreated obstructive sleep apnea can be dangerous. Repeated drops in oxygen levels and frequent sleep disruptions can increase the risk of serious health problems, including high blood pressure, heart disease, stroke, type 2 diabetes, and accidents caused by daytime sleepiness. With proper diagnosis and treatment, these risks can often be significantly reduced.